Understanding Cyst Removal Surgery
At Fall Creek Skin and Health Clinic, we are committed to providing comprehensive care for our patients, ensuring their well-being in both skin-related and general health concerns. One common skin issue that we encounter is the presence of cysts, which may require surgical removal. In this blog post, we aim to shed light on the process of cyst removal surgery to help you better understand this procedure and what to expect.
What is a Cyst?
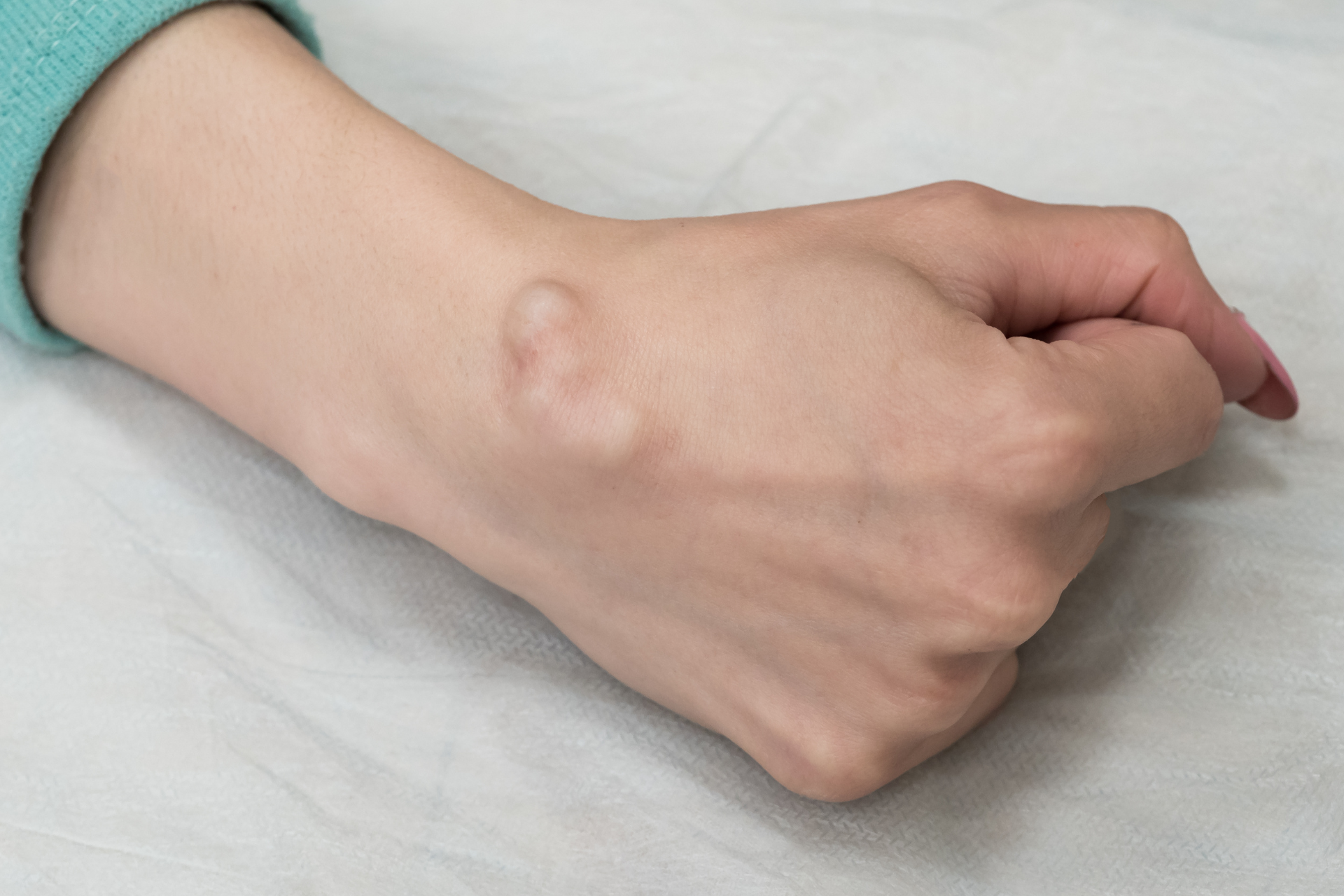
Cysts are fluid-filled sacs that can develop in various parts of the body, including the skin. They can range in size from small to large and are typically non-cancerous. Cysts can form due to a variety of reasons, such as infection, blocked glands, or ingrown hairs. While some cysts may resolve on their own, others may require medical intervention, especially if they become painful, infected, or cosmetically bothersome.
When is Cyst Removal Surgery Necessary?
Cyst removal surgery is often recommended in the following situations:
1. The cyst is causing pain or discomfort.
2. The cyst is infected and requires drainage and removal of the sac.
3. The cyst is cosmetically unappealing and affecting your self-esteem.
4. The cyst is growing rapidly or showing signs of malignancy.
The Cyst Removal Surgery Process
Before the procedure:
Your healthcare provider will conduct a thorough evaluation of the cyst, considering its size, location, and characteristics. They will also review your medical history and any previous treatments for the cyst. You may be advised to stop taking certain medications, such as blood thinners, prior to the surgery to reduce the risk of bleeding.
During the procedure:
Cyst removal surgery is typically performed as an outpatient procedure, meaning you can go home on the same day. The area around the cyst will be cleaned and numbed with a local anesthetic to ensure your comfort during the surgery. In some cases, a small incision may be made to drain the cyst before removal.
The surgeon will carefully remove the cyst along with its contents, making sure to eliminate all traces of the sac to prevent recurrence. The wound may be closed with stitches or left open to heal, depending on the size and location of the cyst.
After the procedure:
Following cyst removal surgery, you may experience some mild pain, swelling, and redness at the surgical site. Your healthcare provider will provide instructions on caring for the wound, including keeping it clean and dry to prevent infection. You may be prescribed pain medication or antibiotics, if needed.
It is essential to attend follow-up appointments to monitor the healing process and ensure that the cyst does not return. In most cases, the recovery period is relatively quick, and you can resume your normal activities within a few days.
Conclusion
Cyst removal surgery is a common and generally safe procedure that can effectively address bothersome or problematic cysts. At Fall Creek Skin and Health Clinic, our experienced healthcare professionals are dedicated to providing top-notch care for patients dealing with cysts and other skin-related issues.
If you have a cyst that concerns you or if you are considering cyst removal surgery, we encourage you to schedule a consultation with our team. We will assess your condition, discuss treatment options, and guide you through the process with compassion and expertise. Your well-being is our priority, and we are here to support you every step of the way.
For more information on cyst removal surgery or to book an appointment, contact Fall Creek Skin and Health Clinic today.
Remember, your skin health is a reflection of your overall well-being, and we are here to help you look and feel your best. Stay informed, stay healthy!